Fewer Side Effects.
Better Results.
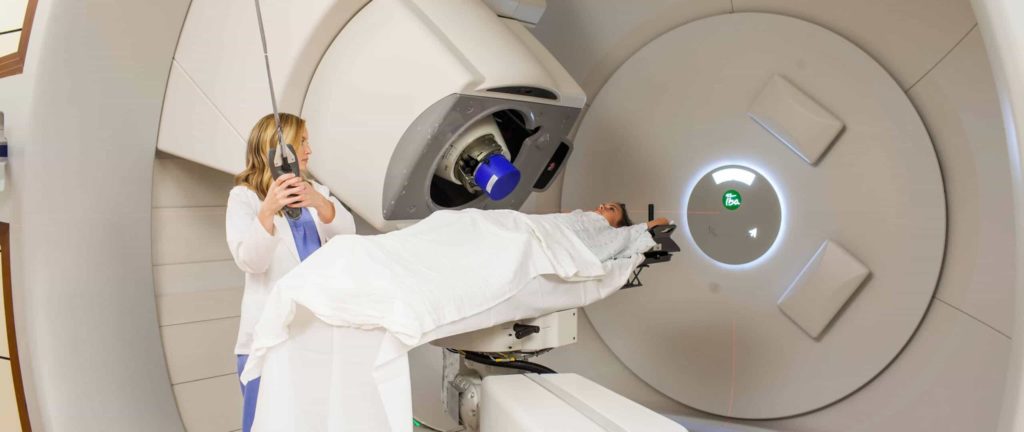
Proton therapy is an advanced form of radiation treatment that suits many types of cancers and tumor types. If a physician recommends radiation therapy as part of a patient’s cancer treatment, proton therapy is likely an option. Unlike common radiation treatments that use X-rays or photons such as IMRT and Cyberknife, protons have a unique physical property that allows radiation oncologists to precisely target a patient’s cancer and stop the protons inside the tumor, avoiding healthy tissue and organs. This decreases the likelihood of undesired and unnecessary side effects. In some cases, proton therapy even offers higher overall survival outcomes and lower recurrence rates than other forms of radiation treatment.
HOW DOES PROTON THERAPY WORK?
Is Proton Therapy right for me?
Proton therapy is a form of radiation treatment that delivers an exact, high dose of radiation to a tumor site while sparing surrounding healthy tissue and organs from damage, reducing the risk of negative side effects during and following treatment. It is non-invasive, non-surgical, and precise, making it an ideal treatment for localized cancers that have not spread to other parts of the body. Proton therapy may be an option for other diagnoses and indications not listed below.

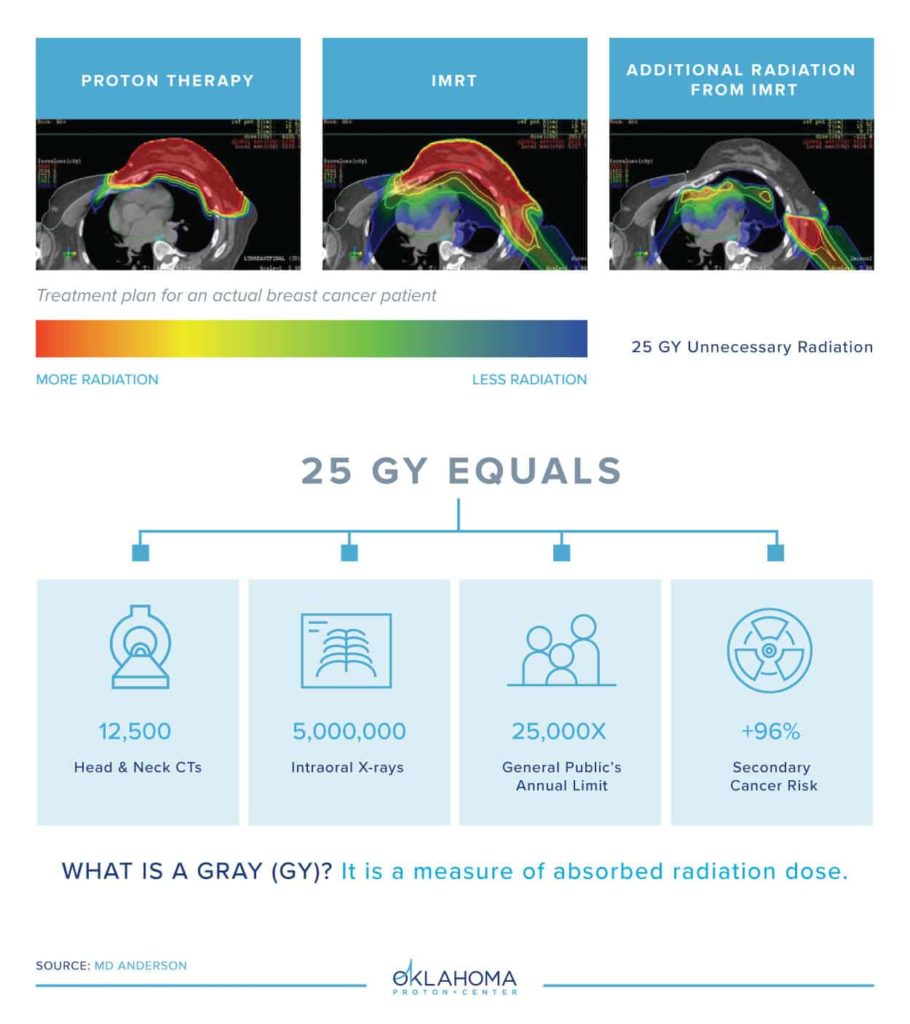
why proton therapy is different:
Protons and X-rays both destroy cancer cells by preventing them from dividing and growing. Protons are energized particles that deliver radiation at exact depths to precisely target tumors. Because protons deposit a majority of the radiation dose at the tumor site and travel no further through the body, the surrounding healthy tissue is spared. X-rays, on the other hand, release their maximum dose of radiation quickly after penetrating the skin, potentially damaging healthy tissue and organs on their way to the tumor site and as they continue to pass through the body.
Find Out if Proton Therapy is Right for You
"*" indicates required fields